The findings, published in Nature Medicine, showed that three of the identified subtypes were the healthiest prediabetes types, while the other three were associated with the most increased risk of type 2 diabetes and secondary diseases.
German scientists have, for the first time, distinguished six different subtypes of prediabetes, a condition that precedes the onset of type 2 diabetes. The research, tracking data from an intensive 25-year longitudinal study, suggests these new subtypes will allow clinicians more precise identification of those patients most likely to develop diabetes.
Type 2 diabetes usually develops quite slowly. As blood sugar levels rise doctors can diagnose patients with prediabetes when those levels are consistently higher than normal, but not high enough to be considered type 2 diabetes.
"For people with prediabetes it has not been possible until now to predict whether they would develop diabetes and be at risk for serious complications such as kidney failure, or whether they would only have a harmless form with slightly higher blood glucose levels but without significant risk," explains Hans-Ulrich Häring, from the University of Tübingen.
The new research, published in the journal Nature Medicine, analyzed 25 years of data from 900 subjects taking part in a longitudinal family heath study. Using a method called cluster analysis the research homed in on six different prediabetes subtypes, each distinguished by different metabolic markers.
"As in manifest diabetes, there are also different disease types in the preliminary stage of diabetes, which differ in blood glucose levels, insulin action and insulin secretion, body fat distribution, liver fat and genetic risk," notes Robert Wagner, first author on the new study.
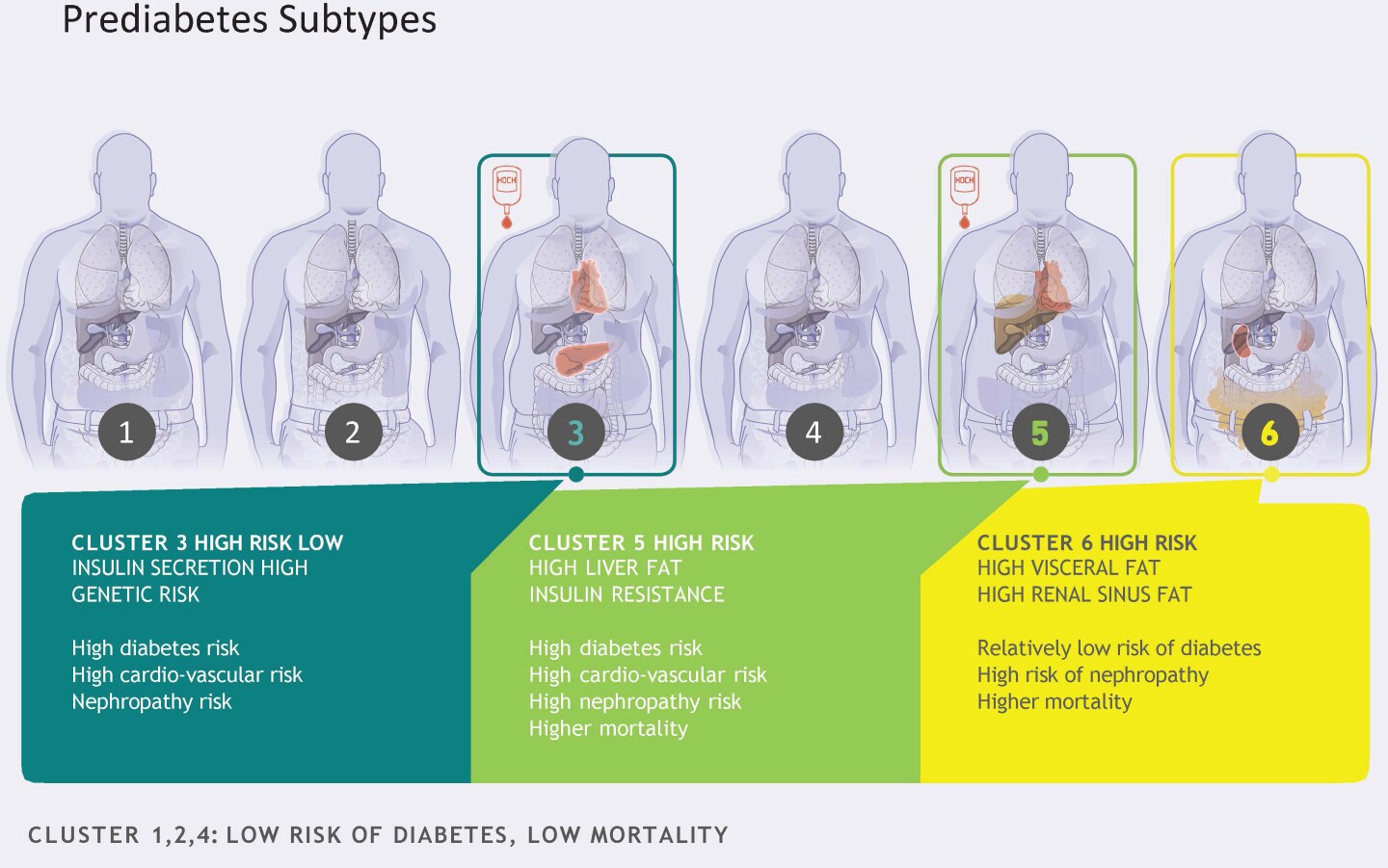
Each of the six prediabetes subtypes described in the study are distinguished by specific metabolic parameters and result in different long-term outcomes. Three subtypes (clusters 1, 2 and 4) are the healthiest types of prediabetes. These subjects present as generally healthy. Cluster 4, for example, encompasses overweight subjects with broadly healthy metabolic markers.
Clusters 3, 5 and 6 were linked to the highest risk of developing type 2 diabetes and secondary diseases. Cluster 5 grouped those subjects with pronounced fatty liver, while cluster 3 grouped those who produced significantly lower levels of insulin.
To further validate these six subtypes, the researchers examined data from another longitudinal study. Called Whitehall II, the UK study tracked the metabolic health of nearly 10,000 subjects for over 20 years. The six subtypes accurately fit that large dataset, affirming prediabetes can be distinguished into separate disease stratifications.
Moving forward the researchers suggest more work is needed to validate these findings before these novel classifications can be utilized by doctors. Martin Hrabě de Angelis, from the German Center for Diabetes Research (DZD), says this work is important in helping catch and treat diabetes before the disease progresses.
"One of the DZD's goals is to develop precise prevention and therapy measures, i.e. the appropriate prevention or treatment for the right group of people at the right time,” says Hrabě de Angelis. “The combination of in-depth clinical and molecular research with state-of-the-art bioinformatics has made this internationally important result possible. The identification of subtypes in the preliminary stages of type 2 diabetes is an important step towards precision medicine in the prevention of diabetes and its complications.”
The new study was published in the journal Nature Medicine.
https://www.nature.com/articles/s41591-020-1116-9
Abstract
The state of intermediate hyperglycemia is indicative of elevated risk of developing type 2 diabetes1. However, the current definition of prediabetes neither reflects subphenotypes of pathophysiology of type 2 diabetes nor is predictive of future metabolic trajectories.
We used partitioning on variables derived from oral glucose tolerance tests, MRI-measured body fat distribution, liver fat content and genetic risk in a cohort of extensively phenotyped individuals who are at increased risk for type 2 diabetes2,3 to identify six distinct clusters of subphenotypes. Three of the identified subphenotypes have increased glycemia (clusters 3, 5 and 6), but only individuals in clusters 5 and 3 have imminent diabetes risks. By contrast, those in cluster 6 have moderate risk of type 2 diabetes, but an increased risk of kidney disease and all-cause mortality. Findings were replicated in an independent cohort using simple anthropomorphic and glycemic constructs4. This proof-of-concept study demonstrates that pathophysiological heterogeneity exists before diagnosis of type 2 diabetes and highlights a group of individuals who have an increased risk of complications without rapid progression to overt type 2 diabetes.
From www.medscape.com
Nyhetsinfo
www red DiabetologNytt